05 Sep What Can Georgia Learn from Buffalo, NY’s Progressive Opioid Solution?
Table of Content
Credit: Family Counseling Services
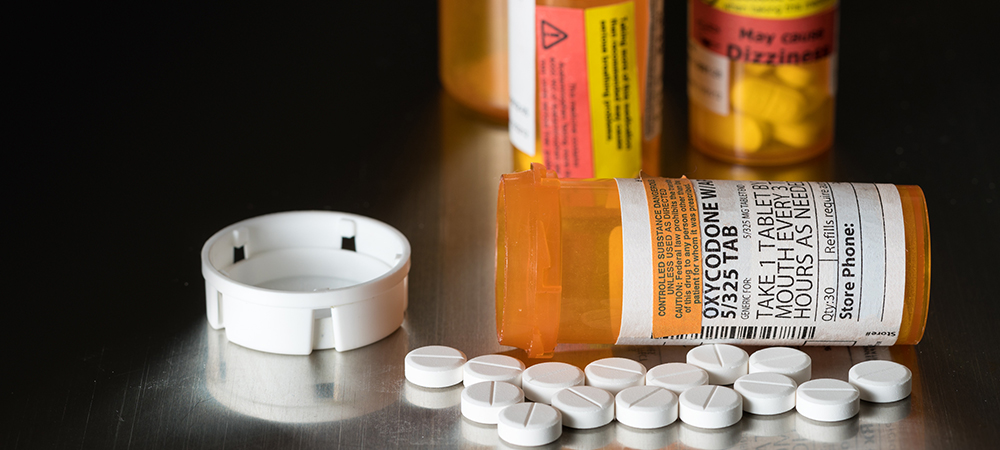
The United States of America consumes nearly 90% of the world’s opioid supply. When taking into account that the US amounts to 4.4% of the world’s population, that statistic isn’t only shocking, it’s gut-wrenching. While the roots of this problem are plenty—and a subject that’s been debated ferociously by opposing parties—let’s focus on a simple fact: we’re consuming too many opioids.
Since the 90’s, opioid prescription in the US basically quadrupled. In 2012 alone 259 million opioid prescriptions were written. That’s enough to basically feed each individual adult living in the US a full canister of addictive medication. This very overprescribing of a drug meant for rare instances in which pain needs to be mitigated has led to an epidemic.
But What Epidemic?
The opioid addiction one. By now you’ve probably heard of it, but if not, let’s break it down for you. In 2015, there were 52,404 lethal drug overdoses. 20,101 were related to painkillers and 12,990 were caused by heroin. This means opiates and opioids (which derive from the same poppy alkaloid) are driving this epidemic and coupled with the fact that prescription rates continue to rise despite FDA regulations, the problem continues to worsen.
But what’s staggering is that the number of lethal overdoses has increased 6 fold since 1999. In not even two decades, we’ve managed to up the death rate of a form of medicine by 600%. Not only that, but at this point in time it’s estimated around 2~million Americans are addicted to some form of opioids. And many of those addicts will go on to become heroin users in the future, due to the depletion of their supply or their addictions becoming to taxing financially to support.
Thus we’re seeing an entirely new wave of heroin users; former patients prescribed opioids that aren’t exclusive to minorities in suburban neighborhoods. That means people are becoming addicted to opioids through their legal use—having been prescribed by a doctor—and then becoming heroin addicts once their fix becomes too difficult to obtain. After all, opioids and opiates allot nearly an identical high. Don’t believe us? Would it shock you to know that currently 4/5 heroin addicts first began with prescription medication? Ten years ago it was 1/5.
Just When We Thought the Problem Couldn’t Get Worse: Enter Fentanyl.
To only add fuel to the fire, fentanyl has hit the market. Fentanyl is an opioid that’s 50 times stronger than heroin and 100 times stronger than heroin. Developed as a medication to assist patients deal with immeasurable amounts of pain—usually prescribed to late-stage cancer patients—now labs in China are replicating the molecular structure of the drug and shipping it here, where dealers mix it into their preexisting drugs (heroin, cocaine, counterfeit prescription pills, etc.).
But this new substance is so powerful we’re seeing mass overdoses across the US, with focuses in certain areas (Maryland, Georgia, and Maine). In fact, we’re now estimating that 50% of opioid overdoses stem from fentanyl. It would be nice to say we have a handle on the problem, but despite the deadly nature of the drug, it’s still in demand and it’s still being imported.
Since drug statistics are always in retro, when the overdose stats start coming through for 2016/2017, they’re going to be heartbreaking.
How Do We Stop This Problem?
The problem is—there’s no easy solution. Opioids aren’t a drug coming from overseas. We can’t just double down our efforts in preventing drug traffic and open up a bunch of treatment homes. The issue with the opioid epidemic is that the problem starts here, in our home, within our own healthcare system.
Of course then, to stop opioid addiction and overdose you’d just stop prescribing opioids altogether. But we’re all aware that there are certain treatments and procedures which are simply not feasible without painkillers. There’s just a price to pay, as one out of every seven people given an opioid for more than five days is going to end up with some form of addiction.
At this place in time, US leaders are finally realizing there’s a serious problem that needs to be addressed. Historically—and since this is such a rapid and recent development—little effort has gone into correcting the problem. At least little in comparison to the efforts needed.
What are Some of Those Efforts?
The CDC’s involvement has begun to change the way doctors are prescribing medication. They’re trying to deepen the common doctor’s knowledge on painkillers and addiction. If there’s a situation where the prescription can be avoided, they’re encouraging professionals to look for substitutes.
Some states are event signing legislation that restricts the amount of time drugs can be prescribed for certain procedures. The idea here is the less exposure a patient has to an opioid, the less likely they’ll become addicted. We’re seeing widely spread efforts to put the drug naloxone in the hands of everyone. Naloxone is a correctional medication used to mitigate the trauma of a heroin overdose (it has to be taken during the overdose).
Donald Trump is currently enforcing much stricter border control, in which we’re seeing huge seizures of counterfeit pills and opiates. Not only that, but he’s also challenging the FDA to promote more anti-abuse drugs and crack down on medication that has proven specifically harmful.
But the thing is national efforts are lacking. We’re seeing a bunch of isolated incidents within certain states where leaders are rising to the occasion (implementing programs, incentivizing doctors, spreading awareness, opening up treatment homes) and while these efforts are supported by national leaders, we have yet to say an installment of something US-wide which will help right the growing problem.
Recently, however, Buffalo, NY has made some very interesting developments in their war against opioid addiction. Interesting enough that they’re turning the eye of leaders who want to help fix this problem, and interesting enough that maybe we all need to learn from them.

Credit: Governor Andrew M. Cuomo
What’s Going on in Buffalo, New York?
Buffalo launched the first ever opiate intervention court program that has been in effect since the beginning of May. In only four months they’ve had impressive results. Their thesis: instead of moving headfirst into the criminal’s prosecution, let’s provide help if their motives or circumstance is brought about by addiction.
Since there’s an average of one overdose death per day in Erie County, the state decided it was time to implement an order directed at saving people’s lives, rather than doubling down on weeding out deviant behavior. Now—whenever anyone is arrested in Buffalo, no matter what the crime that caused the arrest—they will have to go undergo an examination for opiate addiction.
If the screening concludes that they do indeed have an opiate addiction, then their case will be put on hold for a 30-day period while the city provides treatment. There isn’t one unanimous process for each addict; some will be inpatients and other outpatients with daily supervision. Furthermore, instead of treating them and then proceeding with their criminal case, their progress during treatment can directly affect how their case is handled.
The cases will only resume once their program is finished. In short: instead of jailing criminals and immediately rolling into prosecution, Buffalo is giving them resources to treat their addiction and incentivizing them to do so.
This opioid court is the first of its kind, as in a way it actually empathizes with the addict and allows them to first clean up their life before being held accountable for their actions (which they still very much are). The idea is to ‘keep people alive by loving and caring for them.’ That’s something everyone can rally behind.
In today’s line of attack against the opiate epidemic, this is one of the first installments that puts the addict first and identifies their struggles with addiction. Even more to the point of saving lives, being that when a case is pending it’s often a turbulent time for the addict, attorneys see overdoses in this period frequently.
In which case this treatment period isn’t only about helping these addicts long term but protecting them during one of their more volatile periods.
What Can We Learn From this New Court?
Let’s just hit the nail on the head: no one has died. While it’s too new to truly quantify its successes, the fact that every patient who has received treatment is still alive is a statement in itself. As stated previously, many of these patients overdo while their cases are pending. An attorney in Buffalo—in lieu of recent developments—stated that ‘I’ve had eight clients die while their cases were pending.’
At the very least it’s helping curb the fatality rate of this period. It’s also funded partly by a grant. This grant came from the U.S. Department of Justice Bureau and they’ve teamed up with a couple local treatment programs to put the new court in full-effect. The overhead is going towards hiring more staff and space for these addicts (particularly those that are inpatient—meaning it’s quite severe). The overhead also goes towards medicine that assists in the recovery process. What can we learn from this? That there’s way to find money for these platforms… something they all require.
But what we can really learn from this installment is that it’s a new way of fighting opioid addiction: by placing the addict before the substance they’re addicted to. Being that opioids are heavily integrated into our society and rampant in supply, simply doubling efforts to keep illegal drugs out of our country and punish those administering them does relatively nothing for those currently addicted.
Now let’s focus on something different: this new court isn’t the first in the country, nor in a state, but in a county. Let that sink in. A county. While national efforts against opioid addiction are dismal and for the most part entirely absent—something we spoke on in regards to why the epidemic is here in the first place—isolated communities are now taking it into their own hands to the right the problem.
What we can learn is that they’re experiencing successes, addressing the issue with alternative methods, and they’re trying. Truthfully, not only is it Buffalo’s aim to help those struggling with opioid addiction, but they’re also trying to spread awareness to rally more counties with high overdose rates to take action.
And while this court is the first of its kind, it’s not the first progressive and forward-thinking model put into effect. LEAD (Law Enforcement Assisted Diversion) is a program Albany implemented that attempts to help criminals arrested for dismal drug charges. Instead of simply prosecuting them for the crimes committed, similar to Buffalo’s opioid court, they try and assign the criminal to a manager which handles their specific case. Once the case has been assigned, professionals within the vast network that offer services for drug addiction try and provide help in any way they can.
LEAD is now in Ithaca, Orange County, Rochester, Essex County, Brooklyn, Staten Island, and even Buffalo, too. Our final point on the matter: while these new and interactive ways of dealing with opioid addiction are only in certain counties and cities, if we could expand upon these models and implement them nationally then it could make a huge impact. Maybe it’s time for a new paradigm. Buffalo certainly thinks so.
In Conclusion
Solving the opioid problem isn’t straightforward. We have a huge demand for legal opioids in the US and large corporations behind the supply. We can’t rid of them altogether because those that actually benefit from their medicinal use need them. We can’t just close our borders and not let anything in because then pill mills are going to replicate opioids within our borders. And lastly, we can’t just crack down on criminals in hopes that they won’t traffic more drugs within our communities as we’ve seen that it has had little effect.
But what we’re seeing is that we can help those afflicted. Places like Buffalo and the LEAD program have proved that when you put the addict first, rather than trying to tackle the problem at large, improvements are made. Perhaps the entire methodology behind combating the opioid epidemic needs to change: if we starting placing the addict first, we’ll provide mass-help for those struggling, grant the resources to beat addiction, and by default lessen demand for opioids.
As stated previously, this is a complex issue layered in so many variables it’s hard to quantify. The reality is people are dying. Maybe it’s time we focus on them specifically.
Sources:
“New York State’s Opioid Overdose Prevention Program.” NY.gov. 5 Mar. 2019. https://www.health.ny.gov/diseases/aids/general/opioid_overdose_prevention/
Craig, Hannah. “Buffalo Opioid Intervention Court.” NAWJ. 5 Mar. 2019. https://www.nawj.org/uploads/files/midyear_conference/materials/opioid_crisis/buffalo_opioid_intervention_court_brochure.pdf
“To Save Opioid Addicts, This Experimental Court Is Ditching The Delays.” NPR. 5 Oct. 2017. 5 Mar. 2019.



 678-771-6411
678-771-6411

No Comments