04 Sep The Shifting Demographic of Opioid Users in Georgia
Table of Content
The opioid epidemic is here and it’s ugly. Opioids are now the number one killer for people under 30 and account for more deaths annually than auto accidents. Having scaled to a point where it’s no longer ignorable, it has proven its permanence; it’s up to us to change that. Due to a lack of national effort (something we hope to see soon), we’re seeing certain cities and counties rise to the occasion and try and correct the problem themselves. Yet the war against opioids remains vastly out of our control.
To give you a bit more perspective, America consumes 90% of the world’s opioids while only accounting for 4.4% of the world as a whole. We’ve quadrupled our painkiller prescription rate since the early 2000s and the overdose rates scaled at the same rate. It’s rather simple: the more opioids we dumped into our communities the more people became addicted. The more addicts, the more overdoses.
Georgia is one of the states that has been most affected by the opioid epidemic. A statistic that reflects this: from 2000-2014 hospital admissions for opioid overdose in Georgia rose by 1000%. There are a couple reasons behind this impact. For one, Georgia has always been a state with high drug abuse rates. Since they’re in such a prime position for drug smuggling on the East Coast, cartels and drug syndicates use their highways as trade routes.
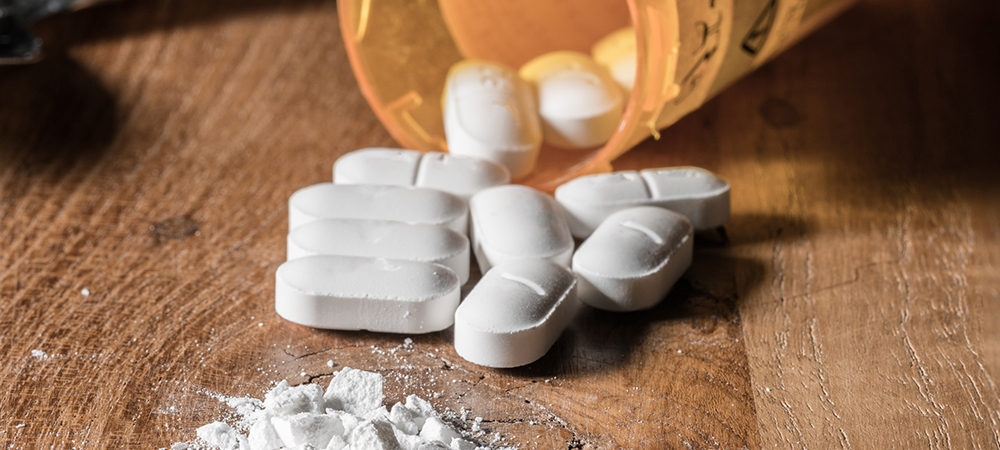
They’re the perfect medium for transportation to NY and allow for major drug outfits from South Carolina, North Carolina, Tennessee, Alabama, and Florida to create a headquarters out of Atlanta. This state is no novice to the world of illegal drugs. From the massive cocaine and crack cocaine push in the 80s, to the heroin boom in the 90s, Georgia has imported and trafficked every drug in America.
You can deduce why they’d also become the stomping grounds for opioids once the market demand rung its siren. Nowadays we’re seeing everything from stolen pills, counterfeit pills, to fentanyl (an opioid 50x stronger than heroin) plow through Georgia. This mass-importation feeds supply and supply is directly linked to overdoses, which have soared as well. Furthermore, one of the other negatives the opioid crisis brought about is a rise in heroin addicts… as if death from opioids wasn’t enough.
Painkillers aren’t necessarily the easiest to come by once you’re addicted. Even doctors once they catch onto an addiction will abstain. The addict will then try to ‘doctor hop’ in hopes of finding an avenue to new prescriptions. But over time they’re flagged or the price of the medication becomes too expensive. Even the street value of a ‘real’ prescription pill can be $20 or $30 bucks a pop. You know what’s cheaper than that? Heroin. It can sell for as little as $10 a bag.
Thus you have opioid addicts fixed on a fix but don’t have the money or the resources to obtain the drug they covet, and the most plausible solution is to switch to heroin. Heroin is an opiate, meaning it’s derived from the same alkaloids of the opium poppy and allots the same high as opioids (pain relief, euphoria).
Historically, opium is the most abused substance in the world—and heroin was and is a big thing in poorer suburban neighborhoods with large ethnic communities, but now we’re seeing an entirely different demographic fall headfirst into addiction: this group of people doesn’t mirror addicts from previous decades.
A Change in Georgia’s Heroin and Opioid Demographic
The rates of heroin and opioid use have always been highest among persons 18-25 years of age, living in urban areas, with an annual household income of equal to or less than 20,000, without Medicaid, and part of a minority group. It’s a sad reality but a reality nonetheless: lower income areas with diverse communities are usually where serious drugs hit the hardest. But now we’re seeing a shift in this phenomenon.
While opioid use quadrupled and heroin doubled across the board in the last decade, the greatest increases (when it comes to percentage) occurred in demographic groups that historically have a much lower abuse rate. It doubled for women and tripled for non-Hispanic whites. Not only that but older ages (25-35) are now seeing a sharp spike in drug abuse as well.
This means that the demographic of drug use (particularly heroin and opioids) is now expanding well outside of where it has formerly been isolated. The disease is spreading so to say, and into white communities thought immune to this class of drugs. Recent findings show there have been significant increases in heroin use in the privately insured and persons with higher incomes bracket. When heroin and opioids are in question, the large divide between the wealthy drug user and the poor one and the man and the woman becomes significantly smaller. In the last decade, we’ve seen a middle ground created. Now 30% of opioid addicts have completed college and 47% of heroin users are high school graduates. And the demographic most at risk isn’t even younger males (white or nonwhite), but it’s adults from 50-69 years of age. Let that sink in. Those most at risk in Georgia are actually well over 40. When coupled with the fact that a few decades ago, senior citizens had to deal with whatever pain (morphine was popular but also heavily monitored) naturally, then it’s easy to expose the source of the problem; opioid prescriptions given to the elderly.
Aside from that, the National Institute of Health just released a statement that said the overdose death within the bracket of white Americans age 23-30 (measured from 1999-2014) rose at a rate that paralleled America’s AIDS epidemic. And while this occurred, overdoses and premature death for minority groups in Georgia declined… and continue to do so.
Thing is—for most other drugs—the demographic remains consistent. Thus we have a shift in Georgia’s opioid and heroin demographic and these consumers are quite unlikely, as they’re the young-middle age white male and female with above average incomes, families, and health insurance.
Why is This Occurring?
Exposure. Aside from certain personality characteristics and uneducated peoples living in areas struck by poverty, it is often environment which serves as a gateway to harder drugs. It’s the same argument used to counter hereditary alcoholism. Some make the case that the exposure to alcoholism and alcohol in a child’s developmental years acclimates the child with the substance abused, which then opens the floodgates to future use.
The same thing can be said about low-income areas notorious for drug use. Being that the youth rises alongside their peers and replicates their example, those of which to say are part of environments that beget crime and drug use, they’re often exposed to said drugs earlier. This early exposure creates a sense of normalcy with the substance at hand, which makes it easier for them to partake in the future.
While this new demographic of peoples outside of minority groups or low-income brackets weren’t exposed to heroin in their earlier ages (removing isolated incidents here) our medical system exposed them to opioids. There should be nothing more alarming for a doctor than a patient returning after a procedure to ask for more painkillers, particularly when the original prescription was more than enough to satisfy the need and then some.
Unfortunately, there is a surplus of these cases. Let’s create a hypothetical. “John” is our quintessential white male. As a youngster, he was humble, responsible, and devoted to his studies. Eventually, he went to college and graduated with a degree. In college, he was exposed to drugs like cocaine and marijuana, but the serious substances were rarely—if ever—in his immediate environment.
Later John meets a lovely woman. He finds a job, too. Eventually, they settle down somewhere decent. Then one summer as John is involved in an accident. Unfortunately, the injury is severe and requires invasive surgery. That’s when he’s first exposed to oxycodone (more commonly known as OxyContin) a heavy-hitting opioid meant for serious pain relief.
John then becomes reliant on said opioid for his pain relief, finishes his prescription, and returns for more. The doctor—under the impression that the treatment was still inducing heavy bouts of pain—fills the prescription a second time. Now John’s chances of becoming an addict are much higher, as studies show they increase by over 30% after the second prescription is given, or after 5 days of use have been met. The addiction wins.
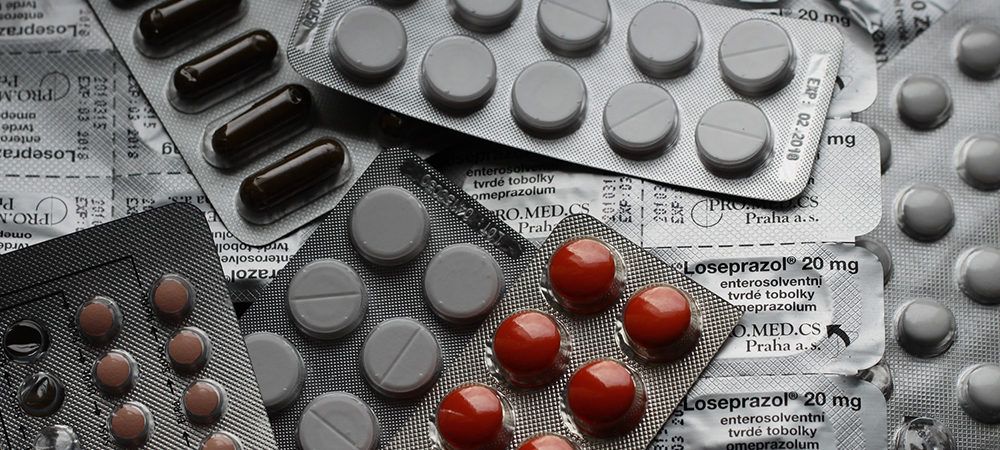
Perhaps he always had a predisposition for addiction. Maybe just an addictive personality? Or there could’ve been internal conflicts settled by the euphoria induced by the opioids, something John wasn’t acclimated with before. The late exposure leads to his addiction and now he ‘doctor hops’ in hopes of a renewed prescription. Eventually, medical professionals catch onto him or his addiction becomes too expensive of a vice to support, so he has to migrate towards illegal drug dealers. From there it’s often a downward spiral and—as studies have shown—often leads to heroin use (hence the entirely different demographic).
As dramatic and poignant as that story is, it’s the reality behind the veil of our opioid epidemic, and it’s happening to our neighbors, teachers, friends, family, loved ones, elderly, esteemed individuals, and breaking through high-income communities. While ‘privileged people’ were able to write off the ‘War on Drugs’ due to a lack of exposure, the shift in paradigm brought about by the opioid epidemic places the problem at their doorstep.
What’s Being Done to Fix the Issue?
At a national level—while plenty of leaders support those makes efforts to right the opioid epidemic—it’s truly the smaller counties and cities that are making the greatest efforts. While the CARA program works to help fight opioid and heroin addiction at a national there, there are some alternative methods that are proving to be more effective.
Before we dive further in, let’s make it known that eradicating the opioid epidemic is a vastly complicated task. The opioid epidemic isn’t exclusive to a drug we’re importing that’s causing mayhem, it’s engrained in the structural flaws of our healthcare system. As if the fact that we consume 90% of the world’s opioid supply isn’t enough, we’re still overprescribing, over producing, and our monitoring programs are nearly useless. Righting this problem begins with the vehicles driving the painkiller industry but tackling its core is an entirely different animal (and an intimidating one).
In which case where we’re seeing the most success is in incidents that put the addict before the drug. Rather than categorizing the drug itself as a threat and devising a solution which rids of it, placing the victim of addiction and empathizing with them is at least beginning to make headway towards a better handle on the problem.
For instance, in Buffalo, New York, if you’re arrested for whatever crime you’re now required to go through a screening process. The purpose: to identify whether or not you’re suffering from an opioid addiction. If the examination exposes your addiction, then your criminal case is put on hold for 30 days and the court provides resources for your recovery. This recovery is either inpatient or outpatient dependent on the severity of the addiction, and the efforts of the criminal within recovery can affect the outcome of their case (huge incentive).
In this way, they empathize with the addict, provide a solution to help them, and yet still continue with the prosecution. This forward and progressive way of thinking is the same sort of core color found in LEAD (Law Enforcement Assisted Diversion) which helps place criminals arrested for low-level drug chargers in the hands of a case manager. These managers then try and find resources and help for the addict.
Then in Georgia, there are multiple platforms and treatment centers working to give these addicts a place to turn. While they haven’t instated an opioid court (like in Buffalo) that very forward way of thinking is starting to seep into their platforms too.
But aside from that, the Trump administration has made a lot of promises they have yet to deliver on. As a whole, we’re waiting for a national movement to combat this issue, as these isolated programs aren’t enough to stop the epidemic. After all, it’s still claiming lives and doing it more so every coming year.
In Conclusion
The war on drugs—something wildly criticized and controversial—is often said to be the war on poverty. This is due to national data which proves low-income urban areas suffer the worst from drug abuse (and just as well benefit from its demand). It’s one of those topics that privileged white America often writes off because it ‘has nothing to do with them.’ There’s a degree of separation, right?
But the opioid epidemic is different, as seen here in Georgia’s evolution of demographic. The exposure of opioids is creating addicts out of a group of peoples historically untouched by drug abuse (dating back to the heroin boom in the 70’s and the cocaine craze in the 80’s).
Georgia as a state is simply a microcosm of the phenomenon occurring across the country. The divide between the historical drug addict and those that were ‘impervious’ to these forces is vanishing. You’d think that alone would turn the eyes of everyone in this country, but America has yet to wake up. But experts say that since we’ve let the problem evolve into what it has become in such a short time, we’re all in for a rude awakening. We’d guess they’re right.
Sources:
“Georgia Opioid Summary.” NIH. Feb. 2018. 13 Mar. 2019. https://www.drugabuse.gov/drugs-abuse/opioids/opioid-summaries-by-state/georgia-opioid-summary
“Vital Signs: Demographic and Substance Use Trends Among Heroin Users — United States, 2002–2013.” Centers of Disease Control and Prevention. 10 July 2015. 13 Mar. 2019. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6426a3.htm
“Opioid Overdose Deaths by Race/Ethnicity” Henry J. Kaiser Family Foundation. 2017. 13 Mar. 2019. https://www.kff.org/other/state-indicator/opioid-overdose-deaths-by-raceethnicity/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D



 678-771-6411
678-771-6411


No Comments